24
Jan
2018
A Day In The Life Of A Child With Severe Hypotonia

The following is a guest post by Krista Metz, a stay-at-home mom to two beautiful little boys, one of which has a disability. She writes about raising a child with hypotonia, mothering through depression, and other amazing feats. You can find her work on The Mighty, Her View From Home, and on All Things Considered: A Blog About Raising a Child With Hypotonia
My son was born with hypotonia.
Before I go on, I’ll explain what that means the best way that I know how. Hypotonia means low muscle tone. I like to tell people to think of it like this: our muscle tone is like a rubber band. For you and I, whose muscles are not affected by hypotonia, our rubber band is pulled tight. For those with hypotonia, their muscles are like a rubber band at rest: loose, overly-relaxed, and not always effective in their movements or purpose.
My son, Roland, came into the world very much hypotonic. My husband and I knew right away that something was “off” about our baby. Aside from his physical presentation (arms and legs always sprawled out, head lag when we lifted him, and hip dysplasia), he had breathing difficulties, which required him to be on oxygen in the NICU for a few days following his birth.
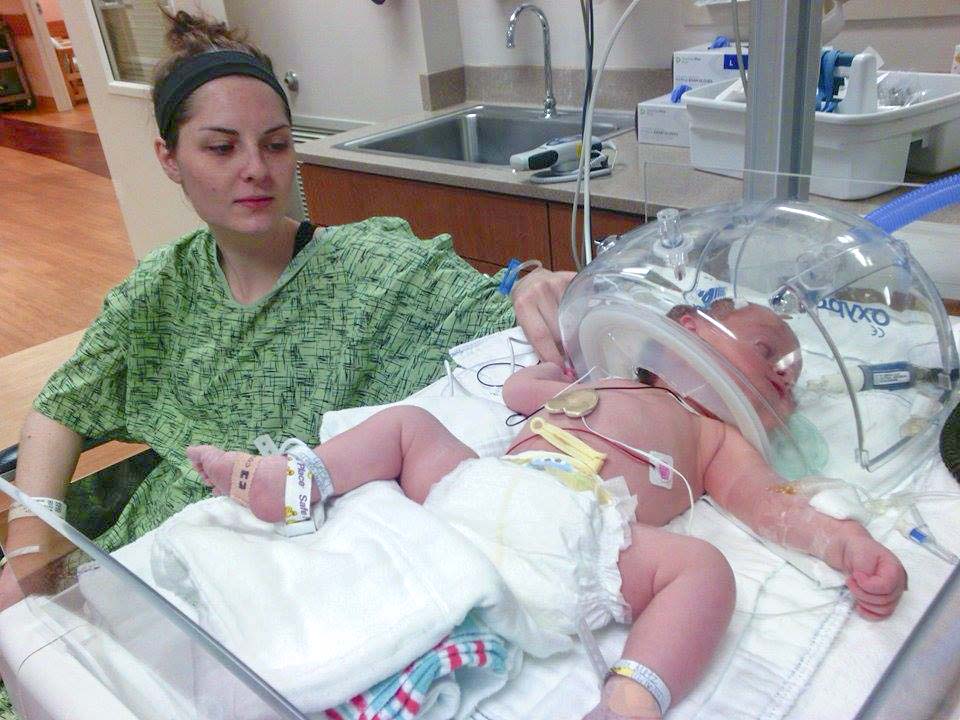
He also had feeding difficulties, due to a weak and uncoordinated sucking reflex. My husband and I found ourselves having to admit Roland to the hospital again, when he was four months old, for failure to thrive. In other words, his body worked so hard to eat that he was actually burning more calories than he was taking in. We were confused about why our baby had so much trouble eating when it came naturally (and without a hitch) to others his age.
Our answer came the day we were admitted. After settling into our room, a doctor came in to perform a physical assessment on Roland. After a lengthy (and almost completely silent) assessment, he said, simply and without hesitation, “Hypotonia.”
“What?” I asked.
“Hypotonia,” he repeated. “I knew it the moment I saw him.”
He went on to explain to my husband and I what this meant (and I can’t be sure that he didn’t give me the rubber band analogy). It was a relief to finally have an answer to the questions in our minds; a diagnosis soothed the growing unsettling feeling in our stomachs and the voice screaming in the back of our minds, something’s not right here! We finally knew the root cause of all of Roland’s struggles.
Fast forward to today. Roland is 3 years old and still has severe hypotonia. After years of searching, we still have no definite answers as to the cause of his hypotonia (but most likely it is due to a rare genetic defect). He cannot roll, sit, stand, or walk. He is g-tube dependent, but is growing like a weed. He can say a few words and loves to babble to any and everyone. Despite all of his limitations, he is a happy boy.
Here is what a typical day looks like for us:
Morning

Just like many other kids his age, Roland goes to preschool. I wake him around 7 so that I can dress him, feed him his breakfast (via g-tube), and drive the 40 minutes to his preschool. He attends a preschool in a neighboring city, one that was specifically built for kids with special needs. He receives occupational, physical, and speech therapy during his three-hour school day.
Roland loves going to school. He plays right alongside his peers–some “typical” peers and some with limitations, as well, because his classroom follows an integrated model–and he does whatever his peers are doing, only adapted to meet his abilities. Some of Roland’s favorite things to do at school are going outside, swinging, reading books, and participating in sensory activities (the messier the better!).

While Roland is at school, I spend this time blogging, scheduling therapies, calling doctors’ offices, ordering feeding supplies, getting Roland’s equipment repaired, and/or grocery shopping. Some days I hang out with him at preschool and meet with his teachers and therapists to see what progress he’s been making and how he’s liking being there.
Afternoon
I pick Roland up from school at 11:30 and feed him again before we make the drive home. We follow a very demanding feed schedule, with Roland receiving something via g-tube every two hours. Some of his peers will gather around while I feed him, amazed by this process. I explain to our audience that Roland has trouble swallowing food, so instead, we put his food right into his stomach with a tube. “This is how Roland eats. Pretty cool, huh?” I say. They will smile and yell “yeah!” Roland smiles back and babbles to them until we are finished and it’s time to go.
Roland almost always falls asleep on our ride home. He gets worn out from his therapies and from playing with his peers. For someone with hypotonia, even the smallest tasks can use up a lot of energy.

Roland will continue his nap at home until it’s time for more therapy. In addition to the therapies he receives at his school, he gets private therapy at our local hospital. To avoid completely exhausting him, we schedule OT and PT on different days, with a speech overlap on one of them. Anyone with a hypotonic child knows how important therapy is; PT and OT strengthen a hypotonic child’s muscles, prevents contractures from developing, and helps them gain skills needed to achieve milestones–or inchstones, as we call them in the hypotonia circle. Often times, it feels like our life is scheduled around therapy, and not the other way around.
Once therapy is done and we are back at home, the rest of Roland’s day is for relaxing and playing (while I try to catch up on housework and take care of Roland’s little brother, who stays at home with my husband during the mornings). Playing, for Roland, looks a bit different than other kids his age. Due to his hypotonia, he struggles with the dexterity and movement required for so many of the toys in his age range. Because of this, I’ve tried to come up with things within his abilities that he can enjoy independently. Some of these include: playing simple games and “reading” books on his tablet, sensory bins, switch-adapted toys, and easily manipulated toys, like cars. Right now, his favorite toy in the world is his spin drum, and he absolutely loves watching Curious George (and anything Curious George-related!). He also loves to “scoot” around on his back, all over our living room.

Evening
While making dinner, I usually put on a movie or tv show for Roland and his little brother or set up some activity in the kitchen for the both of them to engage in while I cook. If Roland is in the kitchen with me, he will beg me to spin him around in his wheelchair by looking at me with puppy-dog eyes and repeating “pin.” He loves any kind of motion–the faster, the better.
After dinner is over, I have Roland choose from a couple books and we read before he goes to bed. He especially likes lift-the-flap books (and they’re great exercise for him).
When both kids are asleep, I finally get time to myself. I use this time to make to-do lists for the next day, set up sensory bins or activities, blog/write, or some other things that I enjoy, like scrapbooking, Netflix-binging, or reading. It would be all-too-easy to spend my free time catching up on housework, laundry, or the hundreds of other chores that I always seem to be behind on. But, as a special-needs mom (and parent in general), I know how crucial self-care is, so I always make time for myself, either at night or some other time during the day.
Our life may look very different from the outside, but we really aren’t that different from other families. We have our own unique challenges, but at the end of the day, my husband and I are simply trying to do the best we can to raise two sons, whom we love more than anything in the world. We want them to be happy and healthy. We just have different ways of achieving this; our son’s disability requires we do things other families don’t have to do. But we have adapted. And we continue to adapt in the face of our unique challenges. Just like every parent does for their child.

Read more personal stories
